All published articles of this journal are available on ScienceDirect.
Nummular Contact Eczema: Presentation of a Pediatric Case
Abstract
The etiopathogenesis of the nummular eczema is not fully known. Various causative factors have been proposed, and among these only a few studies investigate the relevance of contact allergy. Here, we present a case of nummular contact eczema in an 8-year-old allergic to perfumes. Since atopic dermatitis may also present with different clinical phenotypes, among which nummular eczema is quite frequent, the possible significant differences between non-atopic and atopic nummular diseases are considered. Based on the high incidence of contact sensitization in all cases of nummular eczema, it is recommended to perform patch tests for diagnostic-preventive purposes.
1. INTRODUCTION
Nummular eczema, also known as discoid eczema, is a clinical entity characterized by roundish, well-defined margins of the size of a coin [1]. It does not represent a precise etiological entity, and indeed various causative factors, acting individually or in a combined manner, have been identified and suggested as presumable etiological agents. The causal agents most often reported in the literature are nutritional [2, 3], infectious [2, 4, 5] and emotional [6], along with alcoholism [7] and dry skin, especially in old age [8, 9]. Other possible causes are arthropod bites, thermal burns, and varicose veins. In exceptional cases, the disease can be induced by medications [10-12]. Contact irritation and allergy are among the most common etiological factors. In particular, the incidence of contact allergy was studied in various cohorts of patients with nummular eczema [13-17]. From these studies it emerges that exogenous sensitizing agents can complicate (through an altered skin barrier) or initially induce the affliction.
Concerning the correlation with age, nummular eczema is predominantly an adult affection; however, it is observable, albeit with low incidence, even in pediatric age [17-20].
2. CASE
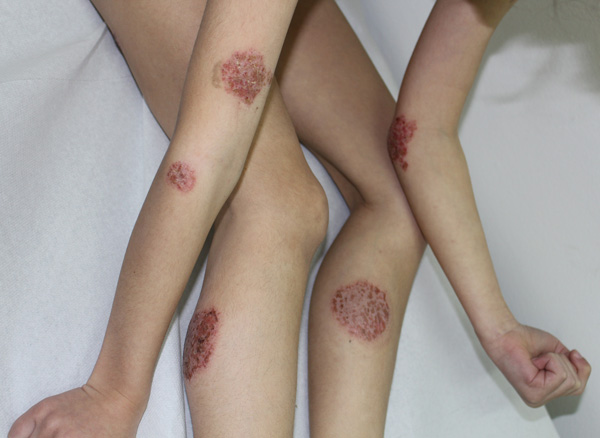
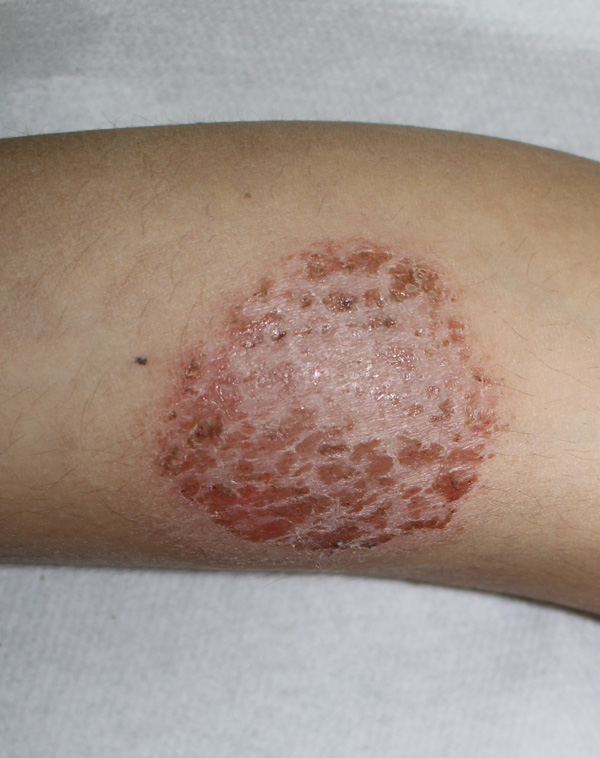
An 8-year-old child presented to us with a pruritic eczematous dermatitis of the limbs. The disease, which occurred 8 months before the observation, first affected the lower limbs, then the upper limbs, with multiple erythemato-papulo vesico crusted lesions in rounded patches of variable size from 2 to 5 cm and well defined margins (Figs. 1, 2). The course of the disease over time had been continuous and progressively worsening, despite the use of emollients and topical antibiotic drugs.
Family history showed atopic dermatitis and allergic rhinitis in the patient's younger sister and an undefined infantile eczema in the mother.
Based on the clinical presentation of nummular eczema, tests were required for possible intestinal infections (parasitological examination of feces), along with skin allergy exams (patch tests) and blood tests (total IgE, RAST).
Patch tests were performed with the standard series SIDAPA (Italian Society of Allergological, Professional and Environmental Dermatology) (Euromedical, Calolziocorte, LC, Italy) and applied on the back with Scanpor® plaster (Norgesplaster, Vennesla, Norway) for 48 hours. Results demonstrated contact allergy to fragrance mix 1 to the reading at D2 and D4 according to the ESCD guidelines (European Society of Contact Dermatitis) (+++ to D2 and D4). The other above mentioned tests turned out negative.
Based on the diagnosis of allergic contact nummular eczema, topical mometasone 0,1% cream (1 application per day) was recommended, along with appropriate preventive measures against perfumed products. Clinical follow-up after 10 days of treatment highlighted resolution of clinical lesions with hyperchromic outcomes. Six-month follow-up did not reveal anything relevant.
3. DISCUSSION
Nummular eczema is an inflammatory skin condition, characterized by multiple eczematous patches of coin sizes with sharp margins. Described by Devergie [21] in 1857, but clinically sketched as early as 1845 by Rayer [22], nummular eczema is not a separate affliction, but a morphological entity in whose onset several factors contribute [17]. While its clinical aspects are clearly defined and known, its pathogenetic mechanism is not. Various factors have been proposed as etiologic agents, of which some are endogenous (dry skin, emotional stress, atopy) and some are exogenous (systemic drugs, alcohol abuse, staphylococcal infections and environmental allergens) [17].
There are scarce studies on the incidence of nummular eczema; in fact, presentations of anecdotal cases prevail in literature. Horn [23] reports an incidence of 7% on all forms of eczema. From our previous study, conducted on 29,323 patch-tested eczematous patients, an incidence of 3.5% emerges [17], as well as a prevalence in males; literature data in this regard are however conflicting: from different observations an equal frequency in the two sexes is seen [24].
Regarding age, nummular eczema is predominantly an adult affliction, with a peak between 20 and 50 years, while, atopic children excluded, it is rarely observable in the first decade of life [17, 18, 25]. In pediatric age, however, the disease occurs more often in females, prevailing in males with advancing age.
The relationship of nummular eczema with atopy is rather controversial. Various studies show no association between discoid eczema and atopy [2, 3, 25, 26], partly based on the observation of low serum immunoglobulin E levels in the first compared to the second [27]. Atopic dermatitis, however, can occur with nummular lesions in both children and adults [18, 28, 29], with a respective incidence of 9% and 12% [18]. Recent studies indicate that nummular lesions represent the most common atypical morphological variant of atopic dermatitis, in pediatric age as well as in adults. In children it is not uncommon to observe coexisting or alternating eczematous nummular lesions along with typical folds involvement [29]. Even in adult atopic dermatitis, nummular lesions represent about 50% of atypical morphological variants of atopic dermatitis [28]. Nummular eczema, therefore, is an important pattern of presentation of atopic dermatitis, regardless of its association to high serum total IgE levels, the presence of specific IgE and the personal or family history of atopy [30].
Between non-atopic and atopic nummular eczema there are several significant differences. Nummular eczema, unlike atopic dermatitis, rarely develops in the first years of life; commonly, it occurs around the age of five. Its natural history is different: cutaneous xerosis is missing and the disease generally does not continue after puberty. Nummular lesions, both in pediatric and adult age, are more exudative, unlike the usually dry and scaling atopic ones, and are less numerous, asymmetric and irregularly shaped and resolve with hyperchromic or hypochromic outcomes (especially in atopics) [31, 32]. The most frequently affected sites are the extensor face of the limbs, while the flexor and the face are usually spared. When nummular eczema is etiologically linked to infections, alcohol abuse or exogenous chemical agents, it resolves quickly without recurrence with specific treatments and prevention.
The incidence of contact allergy in nummular eczema varies from 30.1% to 77.9% of cases [14-16, 33]. In our previous study, conducted on a large patient population, the incidence is of 32.5%, without significant differences between atopic and non-atopic subjects [17]. In subjects with atopic nummular eczema, contact allergy can be interpreted as a “complication” of the pre-existing dermatitis, a consequence of the repeated topical application of drugs and cosmetics. In non-atopic subjects, however, contact sensitization to occupational and / or non-occupational haptens is the “primary” cause of nummular lesions.
CONCLUSION
Many factors have an etiological role in subjects with nummular eczema. Among these, contact allergy is often the primary cause. It is therefore desirable that all cases of persistent nummular eczema, both in atopic and non-atopic subjects, should be patch tested [34].
The differential diagnosis between nummular contact and atopic eczema makes use of various constitutional, anamnestic, environmental and clinical-morphological criteria.
Particularly in pediatric age, the occurrence of nummular lesions in both non-atopic and atopic children is taken into account. In the latter, albeit with a low incidence, the affection can be observed especially in the first few years of life.
ETHICS APPROVAL AND CONSENT TO PARTICIPATE
Not applicable.
HUMAN AND ANIMAL RIGHTS
No animals/humans were used for studies that are the basis of this study.
CONSENT FOR PUBLICATION
Not applicable.
STANDARDS OF REPORTING
This study was carried out in accordance with the principles laid in CARE guideline.
AVAILABILITY OF DATA AND MATERIALS
Not applicable.
FUNDING
None.
CONFLICT OF INTEREST
The authors declare no conflict of interest, financial or otherwise.
ACKNOWLEDGEMENTS
Declared none.


